Asthma, diabetes and cancer. They’re all chronic diseases. But what about obesity? Is it a disease, or something else? According to the American Medical Association and the Canadian Medical Association it is. But not everyone feels that way. The American Heart Association lists obesity as a behaviour (although this may change).
At first glance, the definition of a disease is quite simple. It’s a condition that impairs normal function of one or more parts of the body. But the medical definition of a disease is more complicated. There are definitely changes in biology and metabolism as a result of excess body fat, but the notion to label something a disease has much to do with ensuring people can be treated for it.
And for obesity, there are a number of treatments. There’s behavioural therapy, focusing on eating and activity habits. This might also include the psychological aspects of dealing with obesity. There are also medications for treating obesity along with surgery. While these aren’t sure-fire cures, the same can be said of diseases such as cancer and heart disease. Chemotherapy doesn’t always cure cancer and a coronary artery bypass graft doesn’t cure heart disease.

Bias in Health Care
But just because there are treatments, it doesn’t mean they are easily accessible. It’s well-known people with obesity face bias and ridicule. But this isn’t just limited to the general public. Bias and stigma exist in health care as well. People with obesity report being disrespected by doctors and not taken seriously. This leads to a mistrust in the health care system and avoidance of seeking care. Something that can be detrimental to one’s health later on.
More recently, the Canadian Adult Obesity Clinical Practice Guidelines were released by Obesity Canada. These guidelines are directed to health care professionals. The guidelines received a lot of attention as being progressive and forward thinking. (I had a minor contribution in these guidelines.)
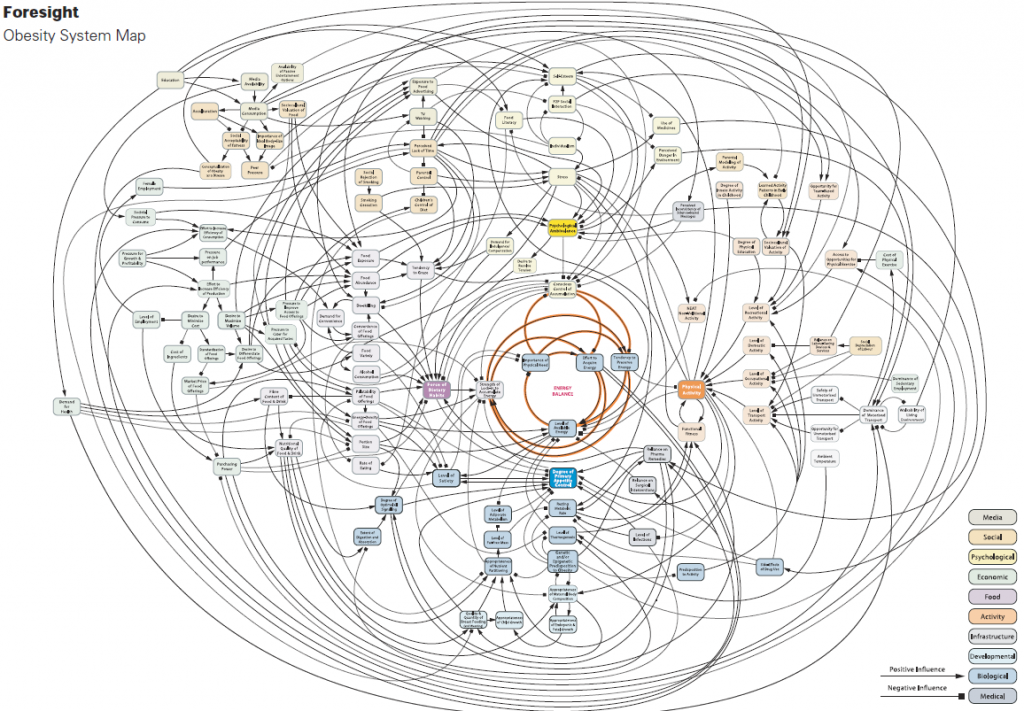
The Latest Guidelines on Obesity
As with previous guidelines, these ones consider obesity a complex chronic disease. This reflects the many factors involved in obesity. From biological and genetic factors to environmental and lifelong experiential factors, obesity is more than just what a person eats and how much activity they get. The guideline writing committee also included people with lived experience with obesity.
However, the guidelines differ from others by separating weight from health. Traditionally, obesity is defined by the body mass index (BMI), a measure of weight over height, greater than 30. However, the BMI was created to study populations. It was never created to be applied to individuals in a medical setting as it is being used now. This is because obesity is a concern of excess body fat, not excess weight. And as I’ve written before, weight is a poor measure of health.
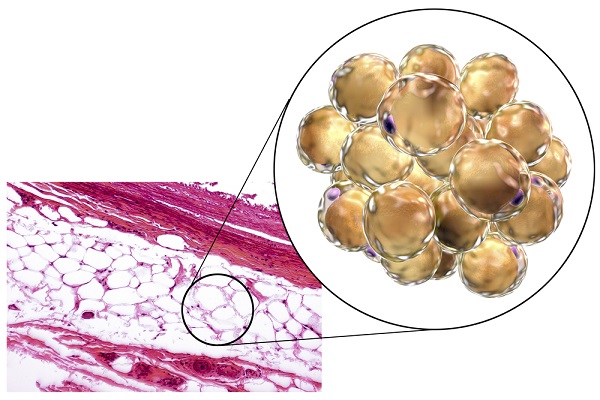
Instead, obesity is defined as “…abnormal or excessive body fat, that impairs health.” Health in this case is determined by an assessment of physical and mental well-being. Therefore, a person could have a high BMI but not be obese if they are healthy. Conversely, it’s possible to have an ideal body size based on BMI but still have a level of body fat that compromises health.
The guidelines also direct the health professional to ask the patient for permission to discuss obesity. This is for two reasons. One, any successful program requires the active and willing participation of the patient. But more importantly, it’s a result of the frequent sigma and bias that people with obesity have experienced throughout their lives and within the health care system.
A key element of the guidelines is the focus on physical health and well-being. Weight loss isn’t the goal. While most suggested treatments may result in weight loss, not all do. Some instead focus on factors related to excess body fat.
A Cure-all for Obesity?
However, these guidelines aren’t a cure-all for obesity. There are many levers of change for managing obesity and health care is just one. It’s clear the environment, and lifestyle within that environment, have a key role in the proportion of obesity in a population. But this is no different from most other chronic diseases. Cancer, asthma and type 2 diabetes all have foundations in the environment, yet are managed predominantly in the medical setting.
Despite this, not everyone was pleased with these guidelines. Some people wrote this would ‘pathologize’ people by calling obesity a disease. And not everyone with obesity would say they have a disease. And fair enough. With obesity having such a prominent appearance-centric quality to it, who wants to look in the mirror and see a diseased person. This adds a layer of complexity that isn’t found in other diseases such as diabetes and atherosclerosis. But for those people who want support from the health care system, these guidelines represent a step forward and call on health professionals to be there for their patients.
If you like this post, don’t forget to subscribe to my blog at the bottom of the page.
Enjoy listening to podcasts? Check out my show How to Health. A podcast about you and your health.

Leave a Reply